
Here's something I tell patients all the time: cataracts are not a death sentence for your vision. They're one of the most treatable conditions in all of eye care. But — and this is the part that matters — you have to catch them at the right time and manage them properly. That's exactly what we do at Eye Medics Optometry in Fayetteville, NC.
I've been evaluating cataracts for over 20 years, and I've seen everything from a 6-week-old infant with a dense congenital cataract to a 78-year-old retired Army sergeant from Fort Liberty who waited too long and lost more vision than he needed to. The common thread? Early detection changes outcomes. Every single time.
We serve patients throughout Cumberland County, including Hope Mills, Spring Lake, Raeford, and the Fort Liberty community. TRICARE is accepted. If you're wondering whether that blur in your vision is a cataract — or if you've already been told you have one and you're not sure what to do next — keep reading.
What Is a Cataract?
Your eye's natural lens sits just behind the iris — the colored part of your eye. In a healthy eye, that lens is perfectly clear, like a clean window. It bends incoming light and focuses it precisely onto the retina at the back of your eye, giving you sharp vision.
A cataract forms when proteins inside the lens begin to break down and clump together, creating a cloudy area. It's a bit like a windshield that's been fogged up from the inside. Light can't pass through cleanly anymore, so your vision becomes blurry, hazy, or washed out.
Most cataracts develop slowly over years. You might not notice anything at first. Then one day you realize you're squinting more at night, or your reading glasses don't seem to be working as well as they used to. That's often the first hint.
A note from Dr. Singletary: "One thing that surprises patients is that cataracts can actually cause a temporary improvement in near vision — what we call 'second sight.' The lens changes its shape as it clouds, which can temporarily make some farsighted patients see better up close without glasses. It sounds like good news, but it's actually a sign the cataract is progressing. Don't be fooled by it."
Types of Cataracts (Including Congenital)
Not all cataracts are the same. Where the clouding forms in the lens determines what type of cataract it is — and that affects the symptoms, the rate of progression, and sometimes who's most at risk. Here's what I see in practice:
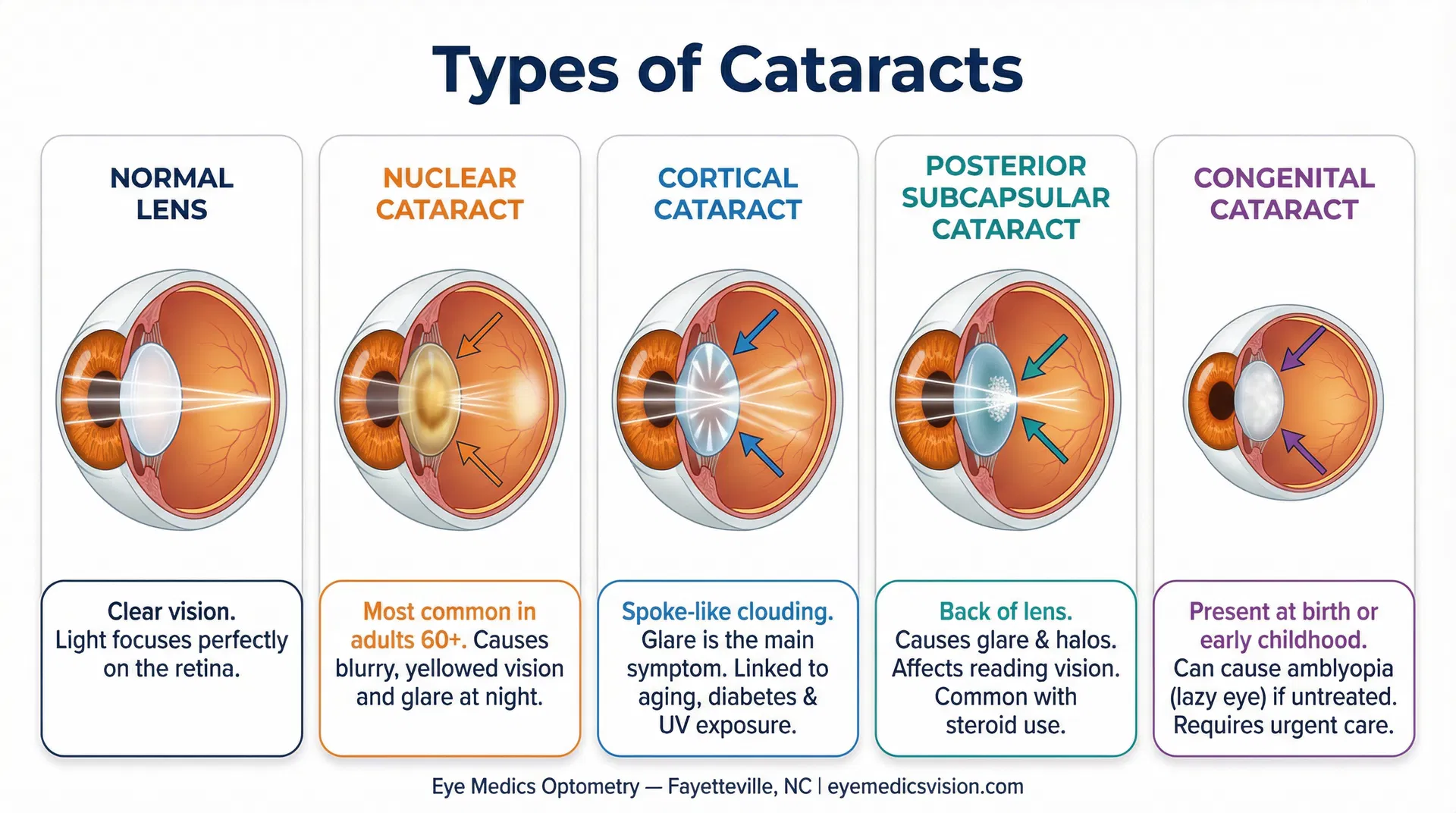
Nuclear Sclerotic Cataract
The most common type. The center (nucleus) of the lens gradually yellows and hardens. Distance vision blurs first. Colors look faded or yellowed. Progresses slowly over years — which is why annual exams matter so much after age 60.
Cortical Cataract
Spoke-like white opacities form in the outer cortex of the lens and grow inward toward the center. Glare — especially from oncoming headlights — is the hallmark symptom. Associated with aging, UV exposure, and diabetes. A 2023 study in Optometry and Vision Science confirmed that cumulative UV-B exposure is a significant independent risk factor for cortical cataract formation.
Posterior Subcapsular Cataract (PSC)
A granular plaque forms at the very back of the lens, directly under the posterior capsule. This type tends to affect younger patients and progresses faster than nuclear or cortical cataracts. Reading in bright light becomes difficult — paradoxically, bright light makes it worse because it constricts the pupil, forcing light through the cloudy area. Long-term steroid use, diabetes, and uveitis are common risk factors.
Congenital CataractInfants & Children
Present at birth or developing in the first months of life. This is the one that keeps me up at night, honestly. A dense congenital cataract blocks the visual pathway during the critical window of visual development — roughly birth to age 7 or 8. If it's not caught and treated quickly, the brain literally stops learning to use that eye, and the result is permanent amblyopia (lazy eye) that can't be fully reversed later. We screen for cataracts at every infant eye exam starting at 6 months. If your pediatrician notices a white reflex in your baby's eye in a photo, that's a red flag — call us immediately.
Symptoms: What to Watch For
Early cataracts often cause no symptoms at all. That's the tricky part. By the time most people notice something is off, the cataract has already been developing for years. Here are the warning signs to pay attention to:
Blurry or hazy vision
That doesn't fully clear with updated glasses
Glare and halos
Around lights, especially at night while driving
Poor night vision
Headlights seem blinding; hard to judge distances
Reading difficulty
Need more light; words seem to swim on the page
Faded or yellowed colors
Blues look gray; whites look yellowish
Frequent prescription changes
Needing new glasses every few months
Interactive
How Cataracts Progress Over Time
Watch how vision changes as a cataract advances through its stages.
EYE MEDICS
Fayetteville, NC · 910.426.3937
123 Westover Hills Blvd
No noticeable symptoms. Cataract detected only on dilated exam. Vision may still be correctable with updated glasses.
Who Gets Cataracts?
The short answer: almost everyone, eventually. By age 80, more than half of all Americans either have cataracts or have had cataract surgery, according to the National Eye Institute. But age isn't the only factor.
Cataract Prevalence by Age Group (United States)
Percentage of adults with visually significant cataracts or prior cataract surgery. Source: National Eye Institute / NEI, 2024.
* Estimates based on NEI epidemiological data. Individual risk varies by health history, UV exposure, and genetics.
In my practice here in Fayetteville, I see a higher-than-average number of patients with early cataracts related to steroid use — both inhaled steroids for asthma and systemic steroids for autoimmune conditions. I also see a lot of diabetes-related cataracts, which tend to develop earlier and progress faster than age-related ones. And with so many active duty and veteran patients from Fort Liberty, I see trauma-related cataracts too — from blast exposure, eye injuries, and radiation.
Risk factors beyond age include: diabetes, prolonged steroid use, significant UV exposure without sunglasses, smoking, family history, prior eye surgery or trauma, and certain metabolic conditions. Cataracts can also be congenital — present at birth — due to genetic mutations, infections during pregnancy (rubella, toxoplasmosis), or metabolic disorders like galactosemia.
How We Evaluate Cataracts at Eye Medics
A cataract evaluation at Eye Medics is part of every comprehensive eye exam — it's not a separate appointment. Here's what we actually do:
Dilated Slit-Lamp Examination
We dilate your pupils with eye drops and examine the lens under our slit-lamp biomicroscope. This lets us see the exact location, density, and type of any cataract — and compare it to previous visits to track progression.
Visual Acuity Testing
We measure how well you see at distance and near, both with and without your current glasses. This tells us how much the cataract is actually affecting your functional vision — which is the key question when deciding about surgery.
Glare Testing
Standard acuity charts don't always capture how bad a cataract is in real-world conditions. We use a brightness acuity tester (BAT) to simulate glare conditions and measure how much your vision drops under bright light — the same conditions you'd face driving at night.
Retinal Evaluation
Before recommending surgery, we need to make sure the retina is healthy. A cataract can mask underlying retinal disease. We use our Optos wide-field retinal imaging system to get a detailed look at the retina, even through a dense cataract.
Surgical Readiness Discussion
If surgery is appropriate, we walk through the process with you — what to expect, which IOL options are available, how TRICARE or Medicare coverage works, and which surgeons we work with in the Fayetteville area.
IOL Options: Comparing Your Choices
When you have cataract surgery, your surgeon removes the cloudy natural lens and replaces it with an artificial intraocular lens (IOL). The IOL you choose affects how well you see — and how much you'll depend on glasses — for the rest of your life. This decision deserves careful thought.
Here's a comparison of the main IOL types available. We discuss these options with every patient before surgery so you go into the operating room knowing exactly what to expect.
| IOL Type | Insurance Coverage | Focus Range | Glasses After Surgery | Best For |
|---|---|---|---|---|
| Monofocal IOL | Standard (TRICARE/Medicare covered) | One distance (usually far) | Reading glasses needed | Budget-conscious patients; those comfortable with reading glasses |
| Toric IOL | Partially covered (astigmatism correction extra) | One distance + corrects astigmatism | Reduced need for distance glasses | Patients with significant astigmatism |
| Multifocal IOL | Premium (out-of-pocket upgrade) | Far, intermediate, and near | Glasses-free for most tasks | Active patients who want minimal glasses dependence |
| EDOF IOL (Extended Depth of Focus) | Premium (out-of-pocket upgrade) | Far and intermediate; limited near | May need reading glasses for fine print | Patients who drive a lot; fewer halos than multifocal |
| Light Adjustable Lens (LAL) | Premium (out-of-pocket upgrade) | Adjustable post-surgery with UV light | Highly customizable outcome | Patients wanting the most precise refractive result |
Source: American Academy of Ophthalmology. Coverage varies by plan. Ask your Eye Medics doctor which IOL is right for you.
The "right" IOL depends on your lifestyle, your other eye's prescription, whether you have astigmatism, and how much you're willing to invest out of pocket. There's no universal answer — but there is a right answer for you, and we'll help you find it.
Cataract Surgery Co-Management
Let me explain how this works, because a lot of patients are confused about who does what.
At Eye Medics, we are optometrists — not surgeons. Cataract surgery is performed by an ophthalmologist, a medical doctor who specializes in eye surgery. What we do is everything around the surgery: the evaluation, the monitoring, the surgical readiness assessment, the referral to a trusted surgeon, and all of your pre- and post-operative care.
This model — called co-management — is the standard of care for cataract patients. According to a 2025 review published in PubMed, optometric co-management of cataract surgery patients improves continuity of care and patient satisfaction, particularly for pre-operative counseling and post-operative follow-up.
The advantage for you: you get a surgeon who does nothing but surgery all day — which means they're very, very good at it — and you get a doctor who knows your complete eye health history managing your recovery. You don't have to start over with someone new.
When to call us sooner rather than later: If you notice a sudden change in vision, a new floater, flashes of light, or a shadow in your peripheral vision, don't wait for your next scheduled exam. These can be signs of a retinal issue — not just a cataract — and they need to be evaluated the same day.
Can You Slow Cataract Progression?
You can't reverse a cataract without surgery — that's just the reality. But you can slow the progression, especially in the early stages. Here's what the evidence actually supports:
Wear UV-blocking sunglasses
100% UV-A and UV-B protection. Every time you're outside. This is the single most evidence-based thing you can do.
Quit smoking
Smokers have 2–3× the cataract risk of non-smokers. The damage is cumulative — quitting at any age helps.
Control your blood sugar
Diabetic cataracts progress faster. Tight glucose control is one of the most important things a diabetic patient can do for their eyes.
Eat your leafy greens
Lutein and zeaxanthin — found in kale, spinach, and eggs — are concentrated in the lens and may help protect against oxidative damage.
Limit steroid use
If you're on long-term steroids for any reason, make sure your eye doctor knows. We monitor for PSC cataracts in these patients closely.
Get regular eye exams
Catching a cataract early means more options. We can monitor it, adjust your glasses, and plan surgery at the right time — not in a crisis.
Free Download
Cataract Readiness Checklist
Not sure if your cataracts are ready for surgery? Download our free checklist — the same questions I walk through with patients in the office. It covers symptoms, functional impact, insurance steps, and what to ask your surgeon.
- 10 questions to assess your functional vision impact
- TRICARE & Medicare pre-authorization checklist
- Questions to ask your cataract surgeon
- What to expect before, during & after surgery
No spam. Unsubscribe anytime.
Related Eye Care at Eye Medics
Frequently Asked Questions
The most common early signs are blurry or hazy vision that doesn't fully clear with glasses, increased glare from headlights at night, colors that look faded or yellowed, and needing more light to read. That said, early cataracts often cause no symptoms at all — which is exactly why a dilated eye exam is the only reliable way to know for sure. We check for cataracts at every comprehensive eye exam at Eye Medics.
References
- 1. National Eye Institute. "Cataracts." Updated November 2025.
- 2. American Academy of Ophthalmology. "What Are Cataracts?" Reviewed by Arjan S. Hura, MD. December 2025.
- 3. Optometry co-management of preoperative and postoperative cataract patients. PubMed. September 2025.
- 4. EyeWiki (American Academy of Ophthalmology). "Cataract." Reviewed by Cullen Ryburn, MD. November 2025.
Medical Disclaimer
This page is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. The information provided here should not be used as a substitute for professional medical advice from a qualified eye care provider. Always consult with a licensed optometrist or ophthalmologist regarding any eye health concerns, symptoms, or treatment decisions.

