
In my practice, dry eye is one of the conditions I see most often — and it's also one of the most underdiagnosed. Patients come in thinking their eyes are just tired, or that they need a new glasses prescription. But when we run the right tests, we find that dry eye is the real culprit. The good news? It's very treatable. At Eye Medics Optometry in Fayetteville, NC, we take a thorough, personalized approach to dry eye — no guessing, no one-size-fits-all solutions.
Whether you live in Fayetteville, Hope Mills, Spring Lake, Raeford, or near Fort Liberty, our dry eye center is here to help you find real, lasting relief. We treat dry eye with a combination of in-office procedures, prescription options, and practical lifestyle changes you can start today.
Not sure if you have dry eye?
Take our free 5-question Dry Eye Self-Assessment — based on the clinical OSDI criteria — and get a personalized severity score in under 2 minutes.
What Is Dry Eye Syndrome?
Dry eye syndrome (also called dry eye disease or ocular surface disease) happens when your eyes don't make enough tears, or when the tears you do make evaporate too quickly. Tears aren't just water — they're a three-layer film made of oil, water, and mucus. When any of those layers breaks down, your eyes can't stay comfortable or clear.
According to the American Optometric Association, dry eye affects tens of millions of Americans — and that number keeps climbing as screen time increases and our indoor environments get drier. It's not just uncomfortable; left untreated, chronic dry eye can damage the surface of your eye and affect your vision long-term.
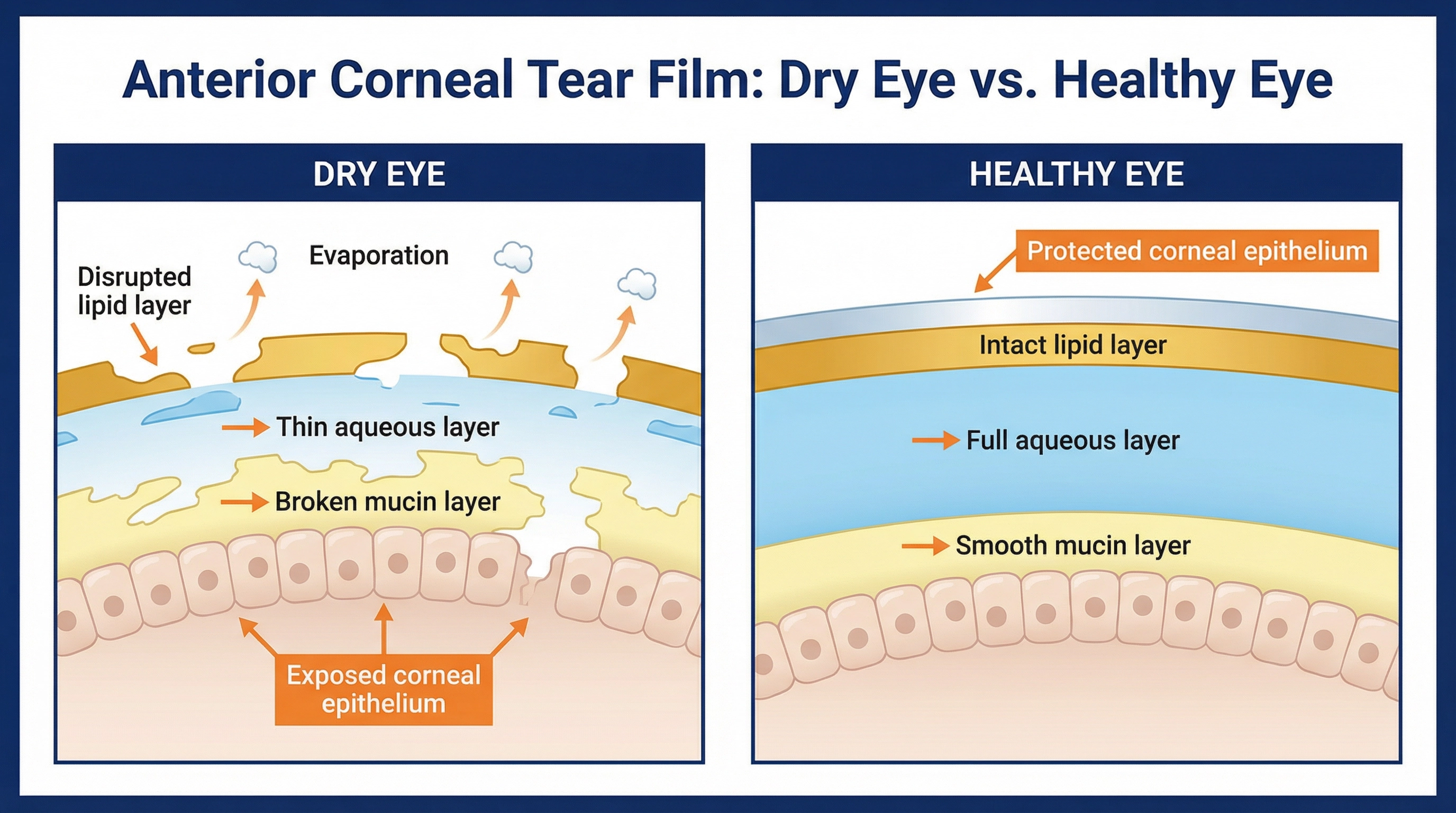
What Causes Dry Eye?
There are two main types of dry eye: evaporative dry eye and aqueous-deficient dry eye. Evaporative dry eye is by far the most common type, and it's usually caused by meibomian gland dysfunction (MGD). The meibomian glands are tiny oil-producing glands along the edge of your eyelids. When they get clogged or stop working properly, the oil layer of your tears breaks down and tears evaporate too fast.
What Causes Dry Eye?
Breakdown by underlying cause (Source: American Optometric Association)
Other common causes of dry eye include:
- Aging — tear production naturally decreases after age 50
- Screen time — blinking less while staring at phones and computers
- Contact lens wear — lenses can absorb tears
- Certain medications — antihistamines, antidepressants, and blood pressure drugs
- Hormonal changes — especially in women during menopause
- Low humidity — dry indoor air from heating and air conditioning
- Autoimmune conditions — such as Sjögren's syndrome or rheumatoid arthritis
- Poor diet — low omega-3 intake and high processed food consumption
Common Symptoms of Dry Eye
One of the most confusing symptoms I see is watery eyes. Patients come in saying, "My eyes can't be dry — they're always tearing up." But that's actually your body's reflex response to irritation. When your tear film breaks down, your eyes produce a flood of low-quality tears to compensate. It's a sign your eye surface is struggling, not that you have plenty of tears.
Common signs include:
If these symptoms sound familiar, it's time to get a proper evaluation. Left untreated, chronic dry eye can lead to corneal damage and long-term vision problems.
How We Diagnose Dry Eye
A proper dry eye diagnosis goes far beyond asking how your eyes feel. We use a comprehensive set of diagnostic tools to identify the exact type and severity of your dry eye — because the treatment depends entirely on the cause:
Tear Osmolarity Testing
Measures the salt concentration of your tears. Higher osmolarity means your tears are more concentrated — a key sign of dry eye.
Meibomian Gland Imaging
High-resolution imaging shows the structure of your oil glands so we can see blockages before they cause permanent damage.
Tear Break-Up Time (TBUT)
We apply a dye to your tears and watch how long it takes for them to break apart. A short break-up time means your tear film is unstable.
Schirmer's Test
A small strip of paper placed at the edge of the eyelid measures how many tears you produce in five minutes.
Slit Lamp Examination
A detailed look at your eyelids, cornea, and tear film under magnification.
This thorough approach means we never guess. We find out exactly what's causing your dry eye before recommending any treatment.
Our Dry Eye Treatment Approach
There's no single treatment that works for everyone. That's why we build a personalized plan based on your specific diagnosis, lifestyle, and goals. Here's a look at the treatments we offer and how they compare:
| Treatment | Best For | Time to Results | Duration of Relief |
|---|---|---|---|
| Artificial Tears / OTC Drops | Mild, occasional symptoms | Instant | Temporary relief |
| Prescription Drops (Restasis®, Xiidra®) | Inflammation-driven dry eye | 3–6 months | Ongoing with use |
| Punctal Plugs | Aqueous-deficient dry eye | Immediate | Months to years |
| Omega-3 Supplements | MGD / tear film instability | 4–8 weeks | Ongoing with use |
| Humidifier / Environment | Dry air / low humidity triggers | Days to weeks | Ongoing |
| Diet & Lifestyle Changes | Systemic inflammation, overall health | 4–12 weeks | Long-term |
Source: Mayo Clinic, American Optometric Association. Individual results may vary.
For most patients, the best results come from combining two or more approaches — for example, punctal plugs plus omega-3 supplements, or prescription drops plus environmental changes at home. We'll walk you through every option and explain exactly why we're recommending what we recommend.
Punctal Plugs
Punctal plugs are one of my favorite tools for the right patient. They're tiny, soft devices — about the size of a grain of rice — that I place in the small opening of your tear duct (called the punctum). By partially blocking that drainage channel, the plug slows down how fast your natural tears leave your eye. The result? More tears on your eye surface, more comfort, and less need for artificial drops throughout the day.
The procedure takes just a few minutes in the office. Most patients don't feel a thing. And if for any reason you don't like them, they can be removed just as easily. A 2025 systematic review published in Contact Lens and Anterior Eye confirmed that punctal plugs significantly improve tear film stability, tear production, and patient-reported symptoms — with non-silicone plugs showing especially strong retention rates.
Who Is a Good Candidate for Punctal Plugs?
- Patients with aqueous-deficient dry eye (low tear production)
- Those who use artificial tears multiple times a day without lasting relief
- Contact lens wearers with chronic dryness and discomfort
- Patients who prefer a non-medication approach
- Anyone whose dry eye hasn't responded well to drops alone
Eye Drops & Prescription Options
Not all eye drops are created equal. Over-the-counter artificial tears can give temporary relief, but they don't address the underlying inflammation that drives most chronic dry eye. For patients with moderate to severe symptoms, prescription drops are often a game-changer.
Restasis® and Cequa® use cyclosporine to reduce inflammation and help your eyes produce more of their own natural tears. Xiidra® works by blocking a specific inflammatory protein on the eye surface — it's particularly effective for patients who notice their eyes feel worst at the end of the day. A newer option, Tyrvaya®, is a nasal spray that activates nerves in your nose to signal your eyes to produce more tears — a completely different approach that works well for some patients.
These prescription treatments typically take 3–6 months to show their full effect, so patience is important. We'll monitor your progress and adjust your plan as needed.
Tip: If you use OTC drops, choose preservative-free formulas. The preservatives in standard drops can actually irritate the eye surface with frequent use — especially if you're using drops more than 4 times a day.
Omega-3 Supplements
I recommend omega-3 fatty acids to a large number of my dry eye patients — and the science is solidly behind it. Omega-3s, especially EPA and DHA found in fish oil, work by reducing the systemic inflammation that contributes to dry eye disease. They also help improve the function of the meibomian glands, which produce the oil layer of your tear film.
A 2023 systematic review and meta-analysis found that omega-3 supplementation significantly improves dry eye symptoms and tear film quality — particularly with higher doses and formulas high in EPA. I typically recommend a high-quality re-esterified triglyceride (rTG) form, which absorbs better than standard fish oil. A dose of around 2,000–3,000 mg daily is what the research supports.
Fatty fish (salmon, sardines, mackerel)
Best food sources of EPA & DHA
Walnuts & flaxseed
Plant-based ALA omega-3s
Chia seeds
Easy to add to smoothies or yogurt
High-quality fish oil supplements
rTG form absorbs best
Results typically take 4–8 weeks. Always check with your doctor before starting high-dose supplements, especially if you take blood thinners.
Environment & Humidity
This is something I talk about with almost every dry eye patient I see — and it's one of the most overlooked triggers. Low humidity is a major driver of evaporative dry eye. When the air around you is dry, your tears evaporate faster than your eyes can replace them. In Fayetteville, this is especially common in winter when the heat is running all day, and in summer when the AC is cranked up.
A 2024 study showed that using a desktop humidifier significantly improved dry eye symptoms and tear film stability in computer users — and even reduced meibomian gland plugging. I recommend keeping indoor humidity between 40–60%. A simple $30–$50 humidifier on your desk or nightstand can make a real difference.
Environmental Changes That Help
- Use a humidifier at your desk and in your bedroom (target 40–60% humidity)
- Point air vents away from your face — direct airflow dries eyes fast
- Wear wraparound glasses or sunglasses outdoors on windy days
- Take regular screen breaks — every 20 minutes, look away for 20 seconds
- Blink fully and consciously when using screens (most people blink 60% less)
- Use a HEPA air purifier if you have allergies or smoke exposure
Diet & Lifestyle
What you eat has a direct impact on your eyes — and dry eye is no exception. Chronic inflammation is a root driver of dry eye disease, and an anti-inflammatory diet can help calm that down from the inside out. This isn't about a strict diet plan; it's about making a few consistent choices that add up over time.
The research is clear: diets high in omega-3 fatty acids and low in processed foods and refined sugars are associated with better tear film quality and fewer dry eye symptoms. A 2019 meta-analysis of 19 clinical trials involving over 4,000 patients confirmed that omega-3 supplementation effectively improves dry eye signs and symptoms — and more recent studies (2023–2025) continue to support this finding.
Foods That Help
- Salmon, sardines, mackerel
- Walnuts & flaxseed
- Leafy greens (spinach, kale)
- Colorful vegetables & berries
- Olive oil
- Plenty of water (stay hydrated)
Foods to Limit
- Processed & packaged foods
- Refined sugars & white bread
- Fried foods
- Excessive alcohol
- High-sodium foods
- Vegetable oils high in omega-6
Self-Care Tips to Manage Dry Eye at Home
While professional treatment is often necessary for moderate to severe dry eye, these daily habits can make a real difference — and they work even better when combined with in-office care:
Use preservative-free artificial tears
Preservatives in standard drops can irritate the eye surface with frequent use. Go preservative-free if you use drops more than 4 times a day.
Apply warm compresses daily
A warm, moist cloth over closed eyes for 5–10 minutes softens eyelid oils and helps unclog meibomian glands.
Take omega-3 supplements
Fish oil or flaxseed oil can improve the quality of your tear film. Look for rTG-form fish oil for best absorption.
Follow the 20-20-20 rule
Every 20 minutes, look at something 20 feet away for 20 seconds to reduce screen fatigue and encourage blinking.
Stay well hydrated
Drink plenty of water throughout the day. Even mild dehydration can reduce tear production.
Use a humidifier at home
Adding moisture to indoor air — especially in winter or with AC running — reduces tear evaporation significantly.
If you wear contact lenses and struggle with dry eye, ask us about specialty contact lens options designed for dry eye patients, including daily disposables and scleral lenses.
Reference Resources
Frequently Asked Questions
In my practice, I see a lot of patients who are surprised to learn that meibomian gland dysfunction — where the tiny oil glands along your eyelids get clogged — is behind about 80% of dry eye cases. When those glands aren't working right, your tears evaporate too fast and your eyes never feel quite right. Screen time, dry air, and certain medications can all make it worse.
Ready for Real Dry Eye Relief?
Patients from Fayetteville, Hope Mills, Spring Lake, Raeford, and Fort Liberty trust Eye Medics for personalized dry eye care. Schedule your comprehensive dry eye evaluation today.
Book a Dry Eye Evaluation
